This really interesting article talks about how many Native American people in Montana struggle to get the care they need. It focuses on people who live in rural and tribal areas where hospitals and doctors are far away and hard to reach. The story explains that problems like long travel distances, lack of money and not enough medical services make it harder for these communities to stay healthy. It also shows how these challenges can lead to worse health outcomes and shorter life expectancy for Indigenous people in Montana, and why this is an ongoing issue that needs more attention.
-

-

Name: Akil McClay
Title: Vice President of Population Health for INTEGRIS Health
Akil McClay is a transformational healthcare executive with more than 15 years of experience advancing value‑based care, operational performance, and enterprise growth across major U.S. health systems. He currently serves as the Vice President of Population Health at INTEGRIS Health, where he leads systemwide revenue strategy, payer partnerships, and value‑based care operations for a $3B health system spanning 16 hospitals. His leadership has driven significant financial turnarounds, multi‑state ACO expansion, and major improvements in quality, risk adjustment, and provider engagement.
Before joining INTEGRIS Health, McClay served as Chief Operating Officer of Population Health for Bon Secours Mercy Health, overseeing four clinically integrated networks and two Medicare Shared Savings Program ACOs across four states. Under his leadership, the organization achieved record-breaking financial performance, including multiple top‑10 national MSSP rankings and more than $150M in shared savings across four years.
McClay’s earlier roles include serving as Director of Alternative Payment Model Operations at Trinity Health, where he directed value‑based operations across 17 CINs in 22 states, generating nearly $300M in shared‑savings revenue; and multiple leadership roles at SSM Health, where he drove systemwide population health initiatives, payer contracting strategies, and care transformation projects.
Throughout his career, McClay has been recognized for building high‑performing teams, scaling innovative value‑based care models, and creating sustainable financial and operational frameworks for health systems managing millions of attributed lives. He holds aMaster of Healthcare Administration from the University of Missouri, aMaster of Neuroscience from Tulane University, and aBachelor of Psychology from Southern University.
Q: Do you believe culture changes the way doctors practice medicine?
Absolutely. Culture shapes how people view health, illness, treatment, and even the healthcare system itself. As a result, physicians inevitably practice medicine through the lens of their own cultural background—and through the cultural expectations of the communities they serve.
In my work in population health, I see how cultural beliefs influence communication styles, patient trust, treatment adherence, and decision‑making. When doctors are culturally aware, they build stronger relationships and deliver more personalized, effective care.
Q; When you hear the term “public health”, what does it mean to you?
To me, public health means creating the conditions for every person to live the healthiest life possible. It’s about looking beyond the walls of the clinic and understanding the broader forces that shape well‑being—housing, food access, education, environment, policy, and community support.
Public health is proactive. It’s about prevention, equity, and systems change, not just treating illness after it appears. As someone working in population health, I see it as the bridge between healthcare delivery and community reality.
Q: What skills do healthcare leaders need to help improve public health?
Healthcare leaders today need a blend of strategic, analytical, and human‑centered skills. Some of the most important include:
- Systems thinking: The ability to understand how policy, care delivery, social services, and community dynamics interconnect.
- Cultural humility: Recognizing that diverse communities have diverse needs and values.
- Data literacy: Using data to identify disparities, guide decisions, and measure impact.
- Collaboration: Working across sectors—education, housing, government, nonprofits—to achieve community‑level change.
- Communication: Explaining complex issues clearly, empathetically, and persuasively.
- Leadership: In public health, it means balancing compassion with strategic execution.
Q: What should young people learn about public health?
I think young people should understand that public health is everywhere. It’s the clean water they drink, the air they breathe, the food safety standards they rely on, and the policies that shape community well‑being.
They should learn that:
- Health isn’t just about biology, it’s shaped by where you live, learn, work, and play.
- Public health is deeply tied to fairness and equity.
- Careers in public health are diverse and meaningful, ranging from epidemiology to community advocacy to health policy.
Most importantly, young people should realize they have power—public health improves when communities get involved and speak up.
Q: What advice would you give students who are interested in healthcare or public health?
I would tell them to stay curious and stay connected to their “why.” Healthcare and public health can be complex fields, but they’re also deeply rewarding.
- Explore broadly: Try different roles—clinical, community‑based, research, policy—to see what resonates.
- Listen to communities: Real understanding comes from hearing people’s stories and experiences.
- Build strong communication skills: No matter what your role, you will need to explain ideas, influence decisions, and collaborate.
- Embrace data: It’s a powerful tool for improving care and reducing disparities.
- Lead with empathy: Technical skills matter, but compassion is what truly transforms health.
-

Clean water is something many people think is normal. In places like the United States, we can turn on the sink and drink water without thinking twice. But in many parts of the world, clean water is still a serious problem. Millions of people do not have access to safe water, and this affects their health and daily lives in many ways.
One reason clean water is still a global problem is because of where people live. In some countries, communities are far away from rivers or water systems. People may have to walk long distances just to get water for drinking or cooking. The water they collect often comes from lakes, rivers, or wells that are dirty. This water can contain bacteria and parasites that make people sick.
Another big issue is poverty. Many countries do not have the money or resources to build good water systems. Pipes, filters, and water treatment plants are expensive and need regular care. When governments cannot afford these systems, people are left with unsafe water. Poor communities are usually the ones hit the hardest, which makes the problem unfair.
Dirty water causes many health problems. People can get diseases like diarrhea, cholera, and typhoid from unsafe water. These illnesses may not sound very serious, but they can be deadly, especially for young children. Many children around the world die each year from water related illnesses that could be prevented with clean water.
Clean water problems also affect education and work. In many places, children spend hours collecting water instead of going to school. Adults may miss work because they are sick or caring for family members who are ill. This keeps families stuck in poverty and makes it hard for communities to improve their situation.
Climate change is making the problem worse. Floods can contaminate water sources, and droughts can dry them up completely. As the climate continues to change, clean water will likely become even harder to find in some regions.
Even though the problem is serious, there is hope. Organizations around the world are working to build wells, improve sanitation, and educate people about clean water. Simple solutions like water filters and protected wells can save lives. Clean water should not be a luxury. It is a basic human need, and solving this problem can help improve health, education, and quality of life around the world.
-

When people think about health, they usually think about going to the doctor when they are sick. While treatment is important, prevention matters even more. Preventing problems before they start can save time, money and stress. It can also help people live longer and healthier lives.
Prevention means making choices that lower the risk of getting sick to begin with. This includes eating healthy foods, exercising, getting good sleep, and going to regular check-ups. These things may seem small, but they make a big difference over time. For example, staying active and eating well can help prevent diseases like diabetes and heart disease. Once someone has these conditions, they often need medication or long-term care, which can be hard and expensive.
Treatment usually happens after a problem has already caused damage. Even the best treatments cannot always fully fix something that has gone wrong. Preventing illness helps avoid pain and suffering that treatment cannot always erase. It is better to stop a problem early than to try to fix it later.
Prevention also helps society as a whole. Fewer sick people means less strain on hospitals and doctors. It also lowers healthcare costs for families and communities. When people stay healthy, they can focus more on school, work, and enjoying their lives.
In the end, prevention is about taking care of yourself before something goes wrong. It may not feel urgent, but it is one of the smartest choices a person can make.
-
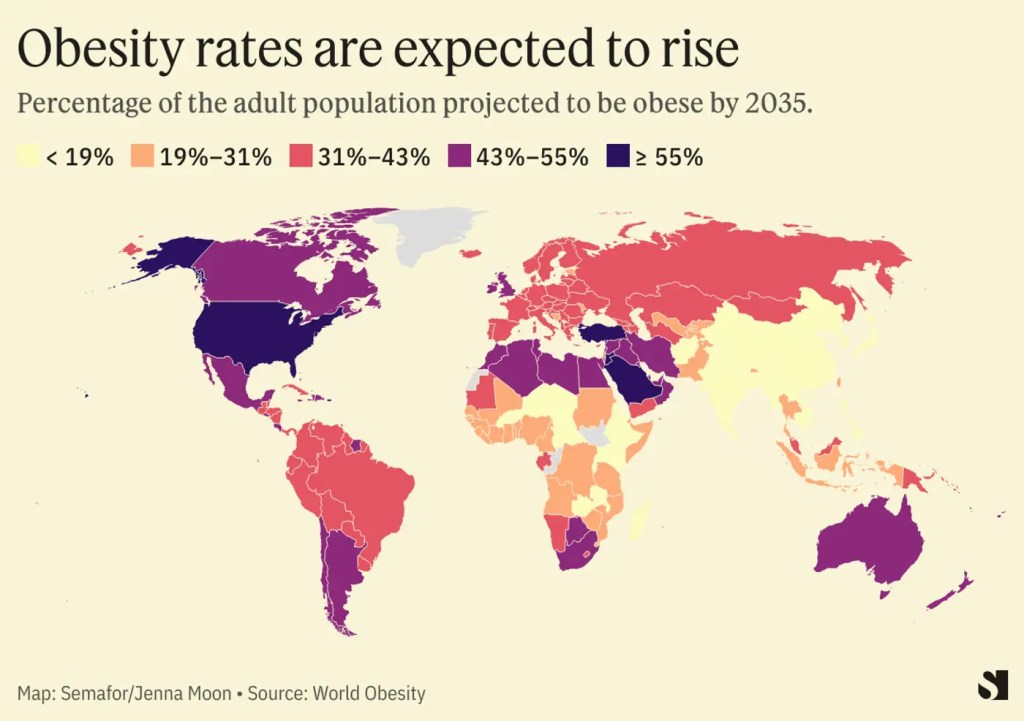
Obesity is a growing health issue around the world, but it does not affect every country in the same way. Obesity is usually defined as having a body mass index (BMI) of 30 or higher, and it increases the risk of diseases like diabetes, heart disease, and stroke.
Globally, obesity rates have risen quickly over the past few decades. The World Health Organization reports that worldwide adult obesity has more than doubled since 1990, and today over one billion people live with obesity. However, where people live makes a big difference. Some countries have very high obesity rates, while others have much lower ones.
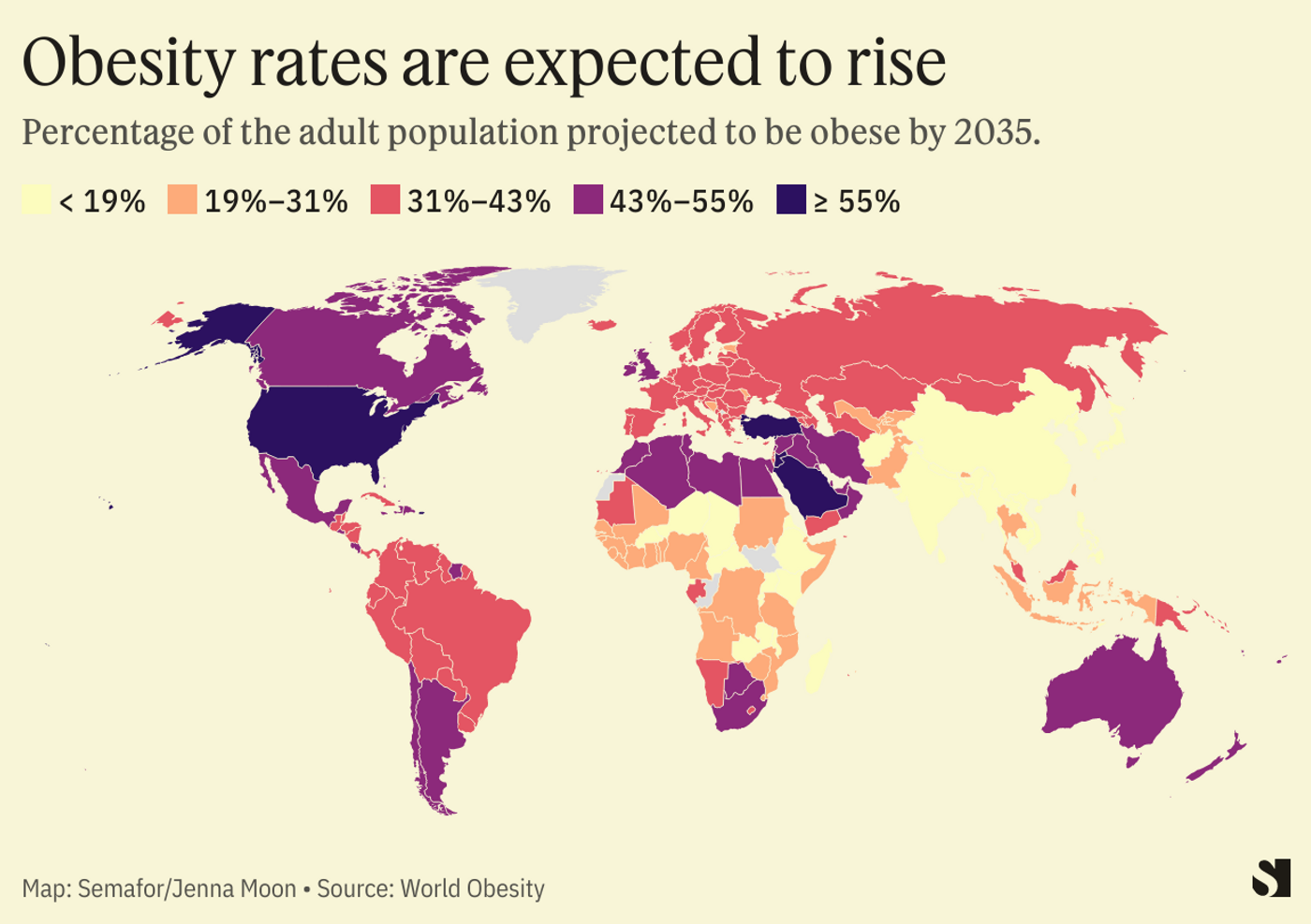
Countries in the Pacific Islands, such as American Samoa, Tonga, and Nauru, have some of the highest obesity rates in the world, with well over half of adults classified as obese. In contrast, many countries in East and Southeast Asia, such as Japan and Vietnam, have much lower obesity rates. High-income countries like the United States, Canada, and the United Kingdom tend to have higher obesity rates than many low-income countries, although this gap is changing over time. The map below shows some of the details by country.
Several factors help explain these differences. In wealthier countries, people often have easier access to processed foods that are high in sugar and fat, and many jobs involve sitting for long periods. In some developing countries, obesity used to be more common among wealthier people, but it is now increasing among poorer populations as diets and lifestyles change.
Overall, obesity is a global problem, but it looks different from country to country. Understanding these differences can help governments and communities create better plans to improve health and prevent obesity in the future.
-

Stress affects the body in more ways than most people realize, and understanding this connection can help people take better care of their health. When someone feels stressed, the body releases hormones like cortisol and adrenaline. These hormones are helpful in short bursts, like when you need to react quickly to danger, but they can cause problems when they stay high for a long time. If someone is dealing with ongoing stress, it can slowly wear down different systems in the body.
One major effect of long term stress is on the immune system. The immune system is supposed to protect the body from infections, but high stress levels can weaken it. This makes it easier to get sick and harder to recover. People who are stressed a lot often notice they catch colds more easily or feel run down even when they are sleeping enough. Stress can also make existing health problems worse, like asthma, stomach issues, or headaches.
Another way stress affects health is through inflammation. Inflammation is the body’s way of fighting off harm, but too much of it can lead to diseases over time. Research shows that chronic stress can increase inflammation, which is linked to conditions like heart disease and diabetes. Stress can also raise blood pressure and make the heart work harder, which adds even more risk.
Mental health and physical health are also connected. When someone feels stressed, they might have trouble sleeping, eating well, or staying active. These habits can slowly create health problems on their own. Even though stress is a normal part of life, it becomes harmful when it builds up without any breaks.
If stress is affecting your health or daily life, it is important to talk with a trusted adult or a healthcare professional who can help you find healthy ways to manage it. What kinds of stress do you notice most often in your daily routine?
-

When people talk about education, they usually focus on things like getting a good job or getting into a good college. But something a lot of people do not think about is how much education actually affects health. The more I learn about global health, the more I realize that school is not just about grades. It can literally change how long people live and how healthy they are.
One of the biggest ways education impacts health is by helping people understand basic information about their bodies. For example, someone who stays in school longer is more likely to know how diseases spread or why clean water matters. They might also know when something feels wrong and that they should go to a doctor. When people do not have access to education, they might not get this kind of knowledge, which can lead to preventable illnesses.
Education also affects health because it influences income. People with more education usually have better job opportunities. Better jobs often mean better access to healthcare, healthier food, and safer living conditions. It is not fair, but it is true that money plays a huge role in health. When families earn more, they can afford things that keep them healthier in the long run.
Another thing I have learned is that education helps communities. When more people in a community are educated, they tend to make better decisions about public health. This can include things like supporting vaccination programs or improving sanitation. It creates a cycle where education leads to better health, and better health helps people stay in school.
Overall, education is one of the strongest tools we have for improving health around the world. It is not just about learning facts. It is about giving people the chance to live healthier and safer lives.